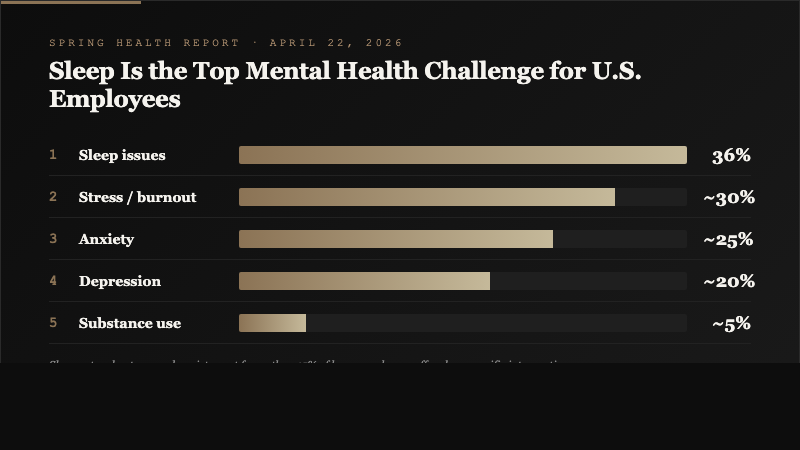
Sleep has quietly become the single most cited mental health challenge among American employees, according to a new Spring Health report published on . Thirty-six percent of employees surveyed named sleep as a primary mental health challenge, edging out stress, anxiety, and burnout, and exposing what the report's authors describe as a significant blind spot in how HR departments structure their well-being benefits.
The finding lands at an inflection point for workplace wellness. Employers have spent the past five years building out mental health programs that emphasized therapy access, teletherapy platforms, and in some cases coverage for prescription medication tied to anxiety and depression. Sleep, a condition that sits at the intersection of physical health, mental health, and environmental factors like shift schedules and commute patterns, has received substantially less structured investment.
Why Sleep Is the Sleeper Issue
The Spring Health report frames sleep as the well-being category most likely to affect job performance, cognitive function, and emotional regulation, yet it is the category employers are least likely to address directly. The logic is intuitive once the data is surfaced. Sleep deprivation impairs decision-making, raises irritability, and compounds the physiological effects of chronic stress. An employee who is sleeping five hours a night is working at a measurable cognitive disadvantage compared with a coworker who is sleeping seven, and the company pays for that in output quality, error rates, and turnover risk.
"Spring Health reports that 36 percent of employees cite sleep issues as a major mental health challenge, highlighting a gap in HR awareness."
Spring Health 2026 Mental Health Report, cited in Sunny Side Sun coverage
The gap is real. A 2024 survey by the SHRM found that roughly 70 percent of large employers offered some form of mental health benefit, but fewer than 15 percent offered specific sleep-related interventions. The ones that did offer sleep programs tended to package them inside broader well-being platforms rather than treating sleep as a stand-alone category with its own outcomes measurement.
What Employers Are Missing
The mismatch between the prevalence of sleep problems and the structure of benefits speaks to how workplace wellness evolved through the 2010s and early 2020s. The mental health conversation in the corporate world was shaped by the pandemic, when therapy access became a frontline issue and several major employers invested heavily in teletherapy platforms including Spring Health, Lyra, and Modern Health. Those platforms solved a real problem, but the pipeline they built runs toward a specific kind of intervention: one-on-one therapy for people who identify themselves as needing mental health support.
Sleep does not fit that model cleanly. Someone experiencing chronic sleep deprivation is unlikely to describe themselves as needing mental health support. They are more likely to describe themselves as tired, busy, overworked, or stressed. The Spring Health data suggests that if those people were offered sleep-specific interventions, including cognitive behavioral therapy for insomnia, structured sleep coaching, or changes to schedule design, a meaningful fraction of them would use those resources.
| Category | Share of employees citing it | Typical employer intervention |
|---|---|---|
| Sleep issues | 36% | Limited, often bundled in broader wellness |
| Stress and burnout | Roughly 30% (range across recent surveys) | Therapy access, PTO policy, EAP |
| Anxiety | Roughly 25% | Therapy platforms, medication coverage |
| Depression | Roughly 20% | Therapy platforms, medication coverage |
| Substance use | Lower single digits | EAP referrals, specialty programs |
Research cited by Spring Health and adjacent workplace wellness studies makes clear that sleep disorders coexist with other mental health conditions at high rates. Insomnia and depression, in particular, have a bidirectional relationship: each worsens the other. An intervention that addresses sleep tends to improve depression and anxiety outcomes as a side effect, which makes sleep-specific investment a relatively efficient use of benefits dollars.
What Actually Works for Sleep
The clinical literature on workplace sleep interventions points to a handful of specific approaches that have demonstrated measurable results. CBT-I, a structured therapy protocol that targets the behaviors and beliefs that sustain chronic insomnia, has the strongest evidence base among adults with persistent sleep problems. Digital CBT-I platforms including Sleepio and Somryst, which deliver the protocol through guided app-based sessions, have run randomized controlled trials showing outcomes comparable to in-person therapy at lower cost per user.
Sleep hygiene education, the more common category of employer intervention, has weaker evidence on its own. Telling employees to keep their bedrooms cool, avoid screens before bed, and stick to consistent sleep schedules produces small effect sizes in the research when offered as stand-alone guidance. The interventions that work are the ones that combine education with behavioral change protocols, structured follow-up, and in some cases adjustments to the work environment itself.
Shift schedule design is the most underused lever on the employer side. Organizations that rotate shift workers on biologically sensible schedules, with forward-rotating shifts and adequate recovery time between shift changes, have lower rates of chronic fatigue and better measured sleep outcomes than organizations that use traditional shift patterns. The healthcare and transportation industries have generated a substantial body of research on this, and the findings translate to other sectors.
The Economics of Sleep in the Workplace
The RAND Corporation has estimated that sleep deprivation costs the U.S. economy roughly $411 billion annually in lost productivity, which amounts to approximately 2.28 percent of GDP. Those numbers are imprecise but directionally consistent with other studies that have placed the economic cost of workplace fatigue at somewhere between $200 and $500 billion annually.
For an individual employer, the math can be made more concrete. A workforce of 10,000 employees with a sleep-deprivation prevalence of 36 percent implies roughly 3,600 people working below their cognitive baseline on any given day. Even conservative estimates of the productivity impact, at 10 to 15 percent reduced output for sleep-deprived workers, translate into meaningful topline effects. A benefits program that addresses sleep for a subset of that population pays back through lower absenteeism, fewer errors, and reduced turnover.
"Sleep is the health behavior most strongly linked to workplace productivity, and it is the one most employers are not addressing directly. That is a benefits design problem, not a biological one."
Workplace wellness research commentary, April 2026

What Companies Are Actually Doing
Some companies have moved in this direction. Google has offered employees access to sleep specialists for more than a decade, and its internal wellness materials treat sleep on the same footing as nutrition and exercise. Microsoft has experimented with meeting-free blocks and adjusted work hours for teams that span multiple time zones. Johnson & Johnson's Energy for Performance program, which has been studied in the research literature, incorporates sleep coaching as a central element.
Outside of a small number of leaders, the broader corporate landscape has been slower to move. The reasons are partly structural: sleep benefits are harder to market internally than therapy benefits because they do not come with the same vocabulary of crisis response or acute need. They are partly cultural: a workplace culture that celebrates long hours and rewards always-on availability is a workplace culture that actively produces sleep deprivation, and fixing the benefits menu without changing the culture produces limited results.
The Spring Health finding may move that conversation. When 36 percent of a workforce names sleep as a primary mental health challenge, the data becomes hard for benefits leaders to ignore. The question is whether the response is meaningful program redesign or a marketing veneer that adds a sleep module to existing wellness platforms without changing the underlying employer behavior.
The Cultural Context
The workplace wellness conversation in 2026 is happening against a backdrop of longer-term cultural shifts in how Americans think about sleep. Public awareness of sleep's importance has grown substantially over the past decade, driven by bestselling books including Matthew Walker's Why We Sleep, increased coverage from outlets like The New York Times and The Atlantic, and the explosion of sleep-tracking wearables from Oura, Apple Watch, Whoop, and Fitbit.
That increased awareness has not consistently translated into better sleep. A 2024 Gallup poll found that 57 percent of Americans said they would feel better if they got more sleep, which is consistent with the Spring Health finding two years later. The gap between knowing sleep matters and sleeping enough is exactly the kind of problem that structured employer intervention can, in principle, address.
The cultural context also includes the post-pandemic shift to hybrid and remote work, which has in some cases improved sleep outcomes by eliminating commutes and in other cases worsened them by extending work hours into what used to be personal time. The data is mixed on the net effect, and company policies on hybrid schedules are still being rewritten across the corporate landscape.
What to Watch
The Spring Health report is likely to accelerate a handful of trends that have been building in workplace wellness. Employer-sponsored sleep programs will expand in visibility, whether through partnerships with digital CBT-I platforms or through in-house coaching offerings. Benefits surveys will start breaking out sleep as a distinct category rather than bundling it inside generic wellness. And the broader conversation about workplace culture, long hours, and the price of always-on availability will get another data point to work with.
For employees, the finding is a permission structure to name sleep as a mental health issue worth addressing, rather than a quality-of-life nuisance to be absorbed. For employers, it is a call to audit their mental health benefits portfolio against the problems employees are actually reporting and to close the gap between the two.
For related coverage, see our reporting on workplace burnout trends and employer responses, on the sleep tracking wearables reshaping personal health data, and on how corporations are restructuring mental health benefits for the hybrid workforce.













